Want help to write your Essay or Assignments? Click here
Acute Tonsilitis
Subjective Data:
Name: J.W. Date: 2/27/2016 Time:
Case ID #: 8008-20164545-015 Age: 35 years old Sex: Female
SUBJECTIVE
CC: Patient feels sick, with multiple symptoms including skin rash, fever, headache, pain in swallowing, sore throat, abdominal pain, nausea and vomiting.
HPI:
The patient is a 35 year old female who presented to the clinic on Saturday, complaining that she has been feeling sharp pain in her abdomen and severe headache. She also notes that she has been experiencing the following symptoms sore throat, pain when swallowing food and nausea plus vomiting.
Patient is accompanied by her 15 year old daughter and 42 year old husband, who bring her to the clinic. J.W. further notes that she has fever and the symptoms began about three days ago, with the sore throat setting in suddenly. This is the first incident that the patient reports to the clinic. The patient notes that she took acetaminophen to relieve the fever and headache, but she decided to consult further treatment once she developed a skin rash.
Medications Currently in Use: Acetaminophen
Past Medical History
Allergies: Allergic to sulfa containing compounds. Had complications after using sulfonamides
Medication Intolerances: Intolerant to sulfonamides and generally sulfa containing drugs
Chronic Illnesses/Major traumas: no major illness/traumas
Hospitalizations/Surgeries: No surgical history recorded; hospitalized once due to pneumonia infection
Family History: No family history recorded on major illnesses; patient’s mum in good health
Want help to write your Essay or Assignments? Click here
Social History
Patient is a casual laborer living with her daughter and husband, plus her 54 year old mum. She takes her lunch from a local cafeteria, but cooks breakfast and supper at her home when she arrives from job in the evening. Her mum helps her cook food, but rarely when she is not present, ill or too tired to cook.
The patient states that she started to suspect food from the cafeteria after a change in management about a month ago. However, she continued to take lunch at the same place, but notes quality had significantly dropped. Also, she had heard a complaint from a regular customer, John, that the food was making him bloat his stomach two weeks ago though the condition disappeared without him attending to hospital.
Review of Systems
General
Positive for fever: No Cardiovascular symptoms. This time she was using acetaminophen
Denies chest pain, palpitations, PND, orthopnea, edema
Has a history of hx pneumonia but negative at the time of admission
Only reports for pain in her abdomen
Skin
Denies bruising, delayed healing, bleeding or skin discolorations. Has no lesion changes or moles but presents with a skin rash
Respiratory
Patient denies cough, breathing regular and symmetrical.
Eyes
Denies eye discharge, no blurred vision, sees clearly without any aid
Gastrointestinal
Reports pain in the abdomen
Ears
Denies pain in ears has no ear discharge, hearing loss, or ringing in ears.
Genitourinary
Denies concerns
Nose/Mouth/Throat
Positive for sore throat
Musculoskeletal
Denies concerns
Breast
Negative history
Neurological
Denies syncope, seizures, transient paralysis, weakness, paresthesia, black out spells
Psychological: Denies depression, suicidal thoughts, irritability,
sleep disturbances, and anxiety
Heme/Lymph/Endo
HIV status, bruising, blood transfusion hx, night sweats, swollen glands, increase thirst, increase hunger, cold or heat intolerance Psychiatric
Denies concerns
Want help to write your Essay or Assignments? Click here
Objective Data
Physical exam is done in the clinic, after which the patient is sent for a lab test out of the clinic. Case is suspected to be upper respiratory bacterial infection particularly streptococcal infection. The following data is recorded from the physical exam;
Vital Signs
Weight 125 BMI 20.7 Temp 101 BP 120/80
Height 170 Pulse 80 Resp 24
General Appearance
Constitutional marked as unremarkable: well developed: well nourished; no acute distress. Vital signs also noted as within acceptable limits. Patient dehydrated. General impression: A&Ox3, nicely dressed, appear appropriate, restless but cooperative, complains of chronic pain in the abdomen and headache
Skin
Skin is black, warm, dry, clean and intact. No lesions noted upon examination. Scarlatiniform rashes noted
HEENT
Head is normocephalic, atraumatic and without lesions; hair evenly distributed.
Eyes: PERRLA. EOMs intact. No conjunctival or scleral injection.
Ears: Canals patent. Bilateral TMs pearly grey with positive light reflex; landmarks easily visualized.
Nose: Nasal mucosa pink; normal turbinates. No septal deviation.
Neck: Supple. Full ROM.
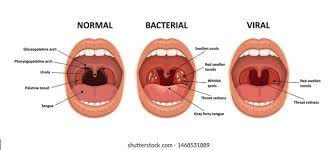
Pharynx redness or exudates over the tonsils noted plus erythema. Beefy red swollen uvula: Anterior cervical Adenitis and Soft Palate Petechiae noted. Teeth and gums are however unremarkable
Want help to write your Essay or Assignments? Click here
Cardiovascular
S1, S2 with regular rate and rhythm. Heart location and apex is normal. No murmurs; no rubs, gallops, or click; femoral pulses normal.
Respiratory
Respiratory unremarkable; respiratory rate and pattern normal; lungs clear to auscultation bilaterally.
Gastrointestinal
Abdomen is soft, non tender and non-distended. No palpable masses. Liver and spleen normal; no hernias; normal bowel sounds, no bloating, only pain in the abdomen noted
Breast
Chest/breast unremarkable, no masses palpitated, no redness
Genitourinary
Bladder is non-distended, no UTI present
Musculoskeletal
Full ROM seen in all 4 extremities as patient moved about the exam room.
Neurological
Speech is clear, Good tone plus Posture erect. Balance is stable; gait normal.
Want help to write your Essay or Assignments? Click here
Assessment
Diagnostics & Lab Tests
Throat smear culture and blood specimen used
Incubation of the culture done for 48 hours before test
The suspected case is streptococcal infection by S. pyogenes or GAS
Positive rapid streptococcal test
Positive results for Antistreptolysin O test
Special Tests
Latex agglutination immunoassay test positive
Want help to write your Essay or Assignments? Click here
Assessment Findings and Plan
Diagnosis:
Patient confirmed to be having Group A Beta hemolytic Streptococcal infection, related acute pharyngitis and acute tonsilitis
Medication:
Penicillin V 500 mg tid for daily 10 days or Amoxicillin 500 mg tid for 10 days
Continue with Acetaminophen till fever completely subsidizes
Amoxicillin is a substitute in the event the patient reports to be allergic to Penicillin
Drugs to be taken orally and in full dosage given by a pharmacist
There are no generic substitutes available
Education
Advice patient to take the following measures:
Use OTC acetaminophen only for fever if relapsing occurs
Wash hands well with soap and water after using bathroom or before eating
Rinse food well and cook properly before eating
Drink water that has been purified or filtered only
Not to smoke or drink alcohol before medication is over and tests negative for GAS
If possible carry packed lunch or change the place she takes lunch from
Want help to write your Essay or Assignments? Click here
Further Notes:
The likely cause of the GAS infection is food from the cafeteria that the patient takes lunch. This, she should refrain from consuming food from the place to avoid a recurrence of the infection. High hygiene standards must be maintained to ensure zero infections to the members of her household, who include her daughter, husband and mum. Also, if convenient to her report the matter concerning the low quality food being sold at the cafeteria to public health offices, for further investigation.
Follow up Schedule
The patient is advised to report to the clinic after a week, for assessment of dosage coverage and progression of the illness. This is to ensure she completes the dosages of all medications in order to eliminate all GAS in her system and avoid development of antibiotic resistance to the Penicillin V given, which results from an incomplete dosage. In this regard, the patient should be advised strongly on the importance of completing her medications, with two follow up meetings being scheduled after a week each.
Want help to write your Essay or Assignments? Click here
Evaluation and Revisions:
The subjective and objective data was collected accordingly but the diagnostics did not cover all possible infections. Since the above are confirmatory of GAS infection, as the cause of the acute pharyngitis and acute tonsillitis, there was deemed no need to conduct tests for other upper respiratory bacteria on the cultures.
This is not only to eliminate the chances of it being a multiple infection case, but also to dictate the medicine given. This revision is necessary alongside a confirmation from the patient concerning her status in connection penicillin allergy, which should dictate the type of antibiotic given. This should be handled accordingly by the pharmacist addressing the prescription.
Metronidazole, Trimethoprim, Tetracyclines and flouroquinolones should not be used for the following reasons. Metronidazole is not effective against S. pyogenes while the patient is allergic to sulfa compounds hence Trimethoprim is contraindicated.
On the other hand, Tetracyclines pose a very high susceptibility to resistance by the bacterial species, that is GAS. Finally, Flouroquinolones are very expensive and have an unnecessary broad spectrum of activity, hence a more specific antibiotic is necessary including the above named plus Azithromycin, Clarithromycin, Clindamycin and various Cephalosporins.
References
Anjos, L. M. M., Marcondes, M. B., Lima, M. F., Mondelli, A. L., & Okoshi, M. P. (2014). Streptococcal acute pharyngitis. Revista da Sociedade Brasileira de Medicina Tropical, 47(4), 409-413.
Camara, M., Dieng, A., & Boye, C. S. B. (2013). Antibiotic susceptibility of streptococcus pyogenes isolated from respiratory tract infections in dakar, senegal. Microbiology insights, 6, 71.
John, L. J., Cherian, M., Sreedharan, J., & Cherian, T. (2014). Patterns of Antimicrobial therapy in acute tonsillitis: A cross-sectional Hospital-based study from UAE. Anais da Academia Brasileira de Ciências, 86(1), 451-457.
Spinks, A., Glasziou, P. P., & Del Mar, C. B. (2013). Antibiotics for sore throat. Cochrane Database Syst Rev, 11.
Want help to write your Essay or Assignments? Click here