End of life care: Are they better off dead?
The most painful event in life is when one loses someone close to them. The people they shared memories with both good and bad. The extent of the hurt often does depend on the situation that they find their loving members. There is a huge difference between a person who dies suddenly and one whom the family members watch while he slowly fades makind end of life care a sentimental factor. The situation also does worsen when the family handles the responsibility of caring for their loved ones as they approach the end of their life. One gets to see the strong personality of their loved one that they cherish fade away replaced by pain (Gillan et al., 2014, p.332).
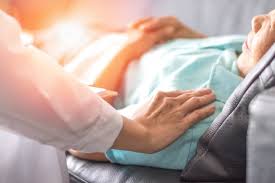
In the dying father and child image, the children are present, and they get to witness the death of their parent. It is a sad event and something that may end up leaving them traumatized or scarred for life. In the picture, one can see one of the children covering their eyes is inferred to mean that they do not want to see their father pass away or they are crying. Tears are a means of expressing our sadness especially in a dreadful situation like death (Murphy 2016 et al., p.254).
It is globally accepted that we will all die at one point in our lives, but no one is ready to see death approach especially when they are not ready (Rowland et al., 2016). As illustrated in the picture, the father is receiving home care as he nears his death. The aspect of patients being taken care of at home arises from two aspects either the hospital has done all they can and informed the patients who decide to spend their last days at home. The second reason deals with the lack of finances, where the family cannot afford to have their patient admitted in the hospital (Tong et al., 2014, p.915).
The family is better placed to understand what their suffering member requires as they near their death from an emotional and spiritual perspective. The emotional perspective is more important to the passing member as they need to feel that someone cares about them. The care they receive solidifies the concept that their lives were worthy in the long run. This is the reason that most members gravitate to their families as they approach their end days (Davies et al., 2014, p.919).
The care is given to the patient often takes different forms depending on their state of mind and disease. In the case of members suffering from chronic diseases like cancer, the pain is often reflected in their eyes and weary bodies. The family members need to assist their loved ones with the help of the medical practitioner to aid the person spend their last days being as comfortable as possible. The aspect of treatment and euthanasia does come into play when discussing the end life care (Wilson, 2013, p. 504).
At times the treatment of people with chronic diseases becomes very expensive to the point that they decide to stop the treatment to save their families the burden of incurring a huge debt (Mathers et al., 2013, p.206). Does the family have a role to play in altering the decision made by the suffering member?
According to the Australian medical health system, the family members have a minimal role in altering the decision of the patient in the case they are still capable of making a sound decision. Despite, this they can discuss with the family member and convince them of continuing with the treatment if they have the finances (Visser, Deliens, and Houttekier, 2014, p.604).
Based on Ewing et al., 2014, p.248, the nursing team has the responsibility from the moral and legal perspective of discussing with the patients the decisions they are to undertake. Once the patient has made their decision, their role comes to an end. Some of the responsibilities that they undertake based on this context are; offering the family members and the patient advice on the treatment available, the cost and what they consider the best option.
The second scenario inferred from the picture focuses on elevating the suffering of both the dying father and the children is euthanasia also referred to as assisted dying. According to Quinlan (2016), euthanasia refers to the intentionally ending the life of a person with the aim of relieving them from the pain that they are undergoing. This is often encouraged in situations where the person is suffering from a chronic and painful disease or is in a coma that is irreversible.
From the legal perspective, the states of New South Wales and Victoria are moving towards drafting legislation that permits euthanasia for Australian citizens (Teno et al., 2013, p.470). The condition stimulated to allow euthanasia is when the patient is suffering an incurable disease that will necessitate them to terminate their life. The decision to give the go ahead for euthanasia lies with the family members and the patients as long as they are above the age of 25 years. Also, the family member at the end of their life needs to have a sound mind at the point of deciding (Morton et al., 2017).
In the case of the dying father and child picture, the love and pain are evident in the way they have gathered around the father. The children love their father and are very young to witness the end of his life. Traumatic events like death often inhibit the effective development of people especially children (Berg, 2014).
Based on the picture the children are very young most of them are below the age of 15 a clear sign that their brain is still developing. I am certain that it is not right but in this case, it is not fair for them to witness such immense suffering of someone they love dearly. Euthanasia would have been a better way to end the pain that they are all experiencing. In this case, the father should have decided to decide to save the elder family member from experiencing any guilt from the incident (Anaf, 2017).
Conclusion
The end of life care is important to the person seeing their life fade away. Most prefer to spend their last days with their families to stay in the hospital. The picture that guides the reflective essay displays this concept. The love and care given by the members enable them to feel comforted as they prepare themselves psychologically for their departure. The end of life care takes different forms as discussed in the essay it can be through euthanasia, hospitalization or home care. One of the common denominators in all the three forms is the advice of the medical practitioner.
REFERENCES
Anaf, J. M. (2017). Voluntary euthanasia laws in Australia: are we really better off dead?. The Medical Journal of Australia, 206(8), 369.
Berg, L., Rostila, M., Saarela, J., & Hjern, A. (2014). Parental death during childhood and subsequent school performance. Pediatrics, peds-2013.
Davies, N., Maio, L., Rait, G., & Life, S. (2014). Quality end-of-life cares for dementia: What have family carers told us so far? A narrative synthesis. Palliative medicine, 28(7), 919-930.
Ewing, G., Grande, G., & National Association for Hospice at Home. (2013). Development of a Carer Support Needs Assessment Tool (CSNAT) for end-of-life care practice at home: a qualitative study. Palliative Medicine, 27(3), 244-256.
Gillan, P. C., van der Riet, P. J., & Jeong, S. (2014). End of life care education, past and present: A review of the literature. Nurse Education Today, 34(3), 331-342.
Mathers, S. (2013). End of Life Care in Progressive Neurological Disease: Australia. In End of Life Care in Neurological Disease (pp. 205-212). Springer London.
Morton, P. G., Fontaine, D., Hudak, C. M., & Gallo, B. M. (2017). Critical care nursing: a holistic approach. Lippincott Williams & Wilkins.
Murphy, B. J. (2016). Voluntary euthanasia laws in Australia: are we really better off dead?. The Medical Journal of Australia, 205(6), 254-255.
Quinlan, M. (2016). “Such is Life”: Euthanasia and capital punishment in Australia: consistency or contradiction?. Solidarity: The Journal of Catholic Social Thought and Secular Ethics, 6(1), 6.
Rowland, C., Hanratty, B., van den Berg, B., Pilling, M., & Grande, G. (2016). Valuing friends’ and family support for end of life cancer care: A national study of the economic costs of informal care giving. Palliative Medicine, 30(6), NP34.
Teno, J. M., Gozalo, P. L., Bynum, J. P., Leland, N. E., Miller, S. C., Morden, N. E., … & Mor, V. (2013). Change in end-of-life care for Medicare beneficiaries: site of death, place of care, and health care transitions in 2000, 2005, and 2009. Jama, 309(5), 470-477.
Tong, A., Cheung, K. L., Nair, S. S., Tamura, M. K., Craig, J. C., & Winkelmayer, W. C. (2014). Thematic synthesis of qualitative studies on patient and caregiver perspectives on end-of-life care in CKD. American Journal of Kidney Diseases, 63(6), 913-927.
Visser, M., Deliens, L., & Houttekier, D. (2014). Physician-related barriers to communication and patient-and family-centred decision-making towards the end of life in intensive care: a systematic review. Critical Care, 18(6), 604.
Wilson, D. M., Cohen, J., Deliens, L., Hewitt, J. A., & Houttekier, D. (2013). The preferred place of last days: results of a representative population-based public survey. Journal of Palliative Medicine, 16(5), 502-508.
Want help to write your Essay or Assignments? Click here.