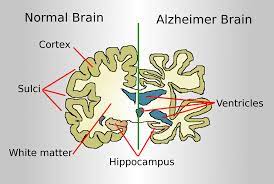
Alzheimer Disease: Genetic Disorders
Question 1
Despite the fact that Federal law aims at protecting people from being discriminated based on their own genes, the Genetic Information Nondiscrimination Act (GINA) has a loophole in that it only apply to health insurance. It does not state anything regarding insurance companies that sell disability, life insurance and long term care insurance. In reality, insurance companies are designed to operate in such a way that people purchase policies but only few percentages of the people insured will use them.
This is to ensure that policies selling are sustainable. However, through genetic testing, people identified with potential risk of developing chronic health condition based on the genetic markers identified are likely to purchase life or disability insurance because they already know that they will develop the chronic disease down the road, making it unsustainable (Feldman, 2012).
The Early onset familial Alzheimer disease (Efad) is a dominant genetic disease, which is caused by single gene mutation. The disease is caused by mutant gene which is inherited from one generation to the other. APOE testing is important health care domain because it aids confirming the disease, or to predict who has the potential of developing the disease in the future.
However, the tests help people to ponder knotty ethical dilemma and life questions. For instance, of one is 25 years old and have a parent who have suffered with the disease, would it be advisable to understand your fate so as to plan and escape it ( Strobel, 2013).
The results of Genetic testing for Alzheimer disease can be devastating if a person carries they carry genes for Early Onset Familial Alzheimer disease. Some people can even decide to end their lives prematurely to avoid facing the health complication associated with the disease. In addition, there is little information on effective treatment options, predictive tests for APOE testing is important in preparing families and patients for decisions that needs to be made such as advance care planning.
It helps in confirming diagnosis, and in developing care plans. The testing informs patient’s family about the diagnosis of Alzheimer disease, and to prepare them financially or have them fill advance directives where necessary. The testing may also facilitate prevention whereby people to make behavior changes such as exercising so as to improve hypertension and other health issues that can negatively impact patient’s cognition (Sheffrin, Stijacic Cenzer, & Steinman, 2016).
Question 2
Most of chronic diseases today are treated using trial and error drug methods. However, pharmacogenomics technological advancement has ensured that physicians are able to match the drugs with right patients, and according to their genetic profile. This ensures that people get the appropriate therapy from the start, and without any complication. This is because healthcare providers are able to prescribe the best drug therapy, thereby speeding their recovery and eradicates potential side effects. Research evidence indicates that this approach can reduce mortality rates by 100,000 and more than 2 million hospitalization rates annually in the USA (Seyerle & Avery, 2013).
Alzheimer disease may occur at any age but its onset is usually at around 40 years. The rate of disease occurrence increases exponentially with age. Alzheimer treatment protocol begins with the diagnosing the patient with Alzheimer disease. The patient baseline functionally and psychiatric state is assessed. If patient condition is mild at diagnosis, the patient begins treatment with acetylcholinesterase inhibitor.
The patient is assessed after 2- 4 weeks, and a stable dosage is established, and the patient is advised to visit the clinic after every 3-6 weeks to continue the treatment. If the patient is not tolerating the medication, the healthcare provider changes to another type of acetylcholinesterase inhibitor until, patient are re-evaluated until the appropriate medication is achieved (Bradford et al., 2011). This protocol highlights that treatment of Alzheimer is basically trial and error as shown in Fig 1 below.
However, the pathogenesis of Alzheimer disease as well as drug metabolism is regulated genetically, and by numerous gene interactions. Alzheimer patients respond moderately to conventional medicine such as donepezil, galantamine, memantine and rivastigmine; with doubtful cost effectiveness. This implies that the healthcare provider must put the following factors into account when choosing the type of cholinesterase inhibitor include a) the dosage, frequency and availability of medication, and b) the number of drugs need to achieve the intended therapeutic dosage. This calls for further assessment of patient’s inherent factors and their ability to deal with medication’s side effects.
The previous pharmacogenomics studies indicated that therapeutic response for this disease is specific to genotype that contains apolipoprotein E. According to these studies, the pharmacogenomics factors may account for 60 to 90% of drug variability in disposition of drugs and in pharmacodynamics. Therefore, modifying the protocol to integrate genomics in management of Alzheimer disease in clinical practice will foster effective therapeutic optimization which will help to develop cost-effective pharmaceuticals, thereby improving drug safety and efficacy (Dua et al., 2011).
References
Bradford, T. W., Onysko, M.K., Stob, C., Hazlewood, K. (2011). Treatment of Alzheimer disease. American Family Physician 2011 retrieved from http://www.aafp.org/afp/2011/0615/p1403.html
Dua, J., Gupta, A., Pachuari, K., Dewangan, S. (2011). Pharmacogencomics- a boon for chronic disease. International journal of Pharma and Bio Sciences 2(2); B- 424
Feldman, E. A. (2012). The Genetic Information Nondiscrimination Act (GINA): Public Policy and Medical Practice in the Age of Personalized Medicine. Journal of General Internal Medicine, 27(6), 743–746. http://doi.org/10.1007/s11606-012-1988-6
Seyerle, A. A., & Avery, C. L. (2013). Understanding Genetic Epidemiology: The Potential Benefits and Challenges of Genetics for Improving Human Health. North Carolina Medical Journal, 74(6), 505–508.
Sheffrin, M., Stijacic Cenzer, I., & Steinman, M. A. (2016). Desire for predictive testing for Alzheimer’s disease and impact on advance care planning: a cross-sectional study. Alzheimer’s Research & Therapy, 8, 55. http://doi.org/10.1186/s13195-016-0223-9
Strobel, G. (2013). Early onset familial AD: Genetic testing and counseling for Early Onset Alzheimer Disease. Retrieved from http://www.alzforum.org/early-onset-familial-ad/diagnosisgenetics/genetic-testing-and-counseling-early-onset-familial
Want help to write your Essay or Assignments? Click here